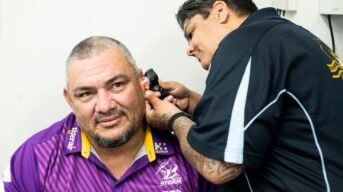
Royal Commission hearing on health and cognitive disability
Below are daily updates form the Sydney hearing provided by Jim Simpson, our Senior Advocate.
Read an Easy Read version of this page
Day nine – “Treat me as a person first and foremost.”
The Royal Commission hearing on health started as it began, listening to a person with disability.
Robert Strike AM was the co-founder of Self Advocacy Sydney in 1986. He has also been on the board of CID since then, and has twice spoken at the United Nations.
Robert talked about how to overcome challenges to communication between people with intellectual disability and doctors. “We are great trainers in how to communicate with us.” He told Commissioners that Easy Read really helps people with intellectual disability understand written information.
Robert said “Treat me as a person first and foremost.”
Earlier, parent Jo Abi spoke of the great challenges she has faced getting a diagnosis for her two sons with autism and getting the right mental health treatment. She emphasised the need for broad community change. “All the treatment is focused on fixing my kids, not fixing the world so they can be who they are,” she said.
The Commission also heard from the mothers of previous witnesses Kylie Scott and Tara Elliffe. They complained of medical assumptions that women should have prenatal testing and then terminate a foetus with Down Syndrome. They said parents should have choice, but should also be given full and balanced information. Both mothers spoke very positively about the GPs their daughters now have, and about how their daughters are in charge of their own health care with support when needed.
Chief Commissioner Ronald Sackville closed the two-week hearing emphasising the power of the evidence, especially the evidence from people with disability and their families. He repeated his opening statement that the neglect and abuse experienced by people with cognitive disability in the health system should shock the nation.
The Royal Commission will be carefully considering what recommendations it should make out of the hearing.
Commissioner Sackville kindly acknowledged the contributions to the hearing of CID, including our advice on how to make the hearing room a more comfortable environment for people with disability. He also emphasised the crucial role of individual and systemic advocacy.

Day eight – Greg Hunt commits $6.5m to health of people with intellectual disability
Before the Royal Commission hearing yesterday, federal Health Minister Greg Hunt committed $6.5 million to initial action on improved GP care for people with intellectual disability. This money will go to the Primary Care Enhancement Program, which will work with GPs and other primary health services improve their skills and focus on people with intellectual disability. Four lead Primary Health Networks (PHNs) will be funded for four years with a view to national rollout across all PHNs.
At the Royal Commission, representatives from the federal Department of Health emphasised the Department’s commitment to finalising the National Roadmap for Improving the Health of Australians with Intellectual Disability. They agreed that this should include, for example, promoting much higher take-up by GPs of Medicare annual health assessments for people with intellectual disability.
After many years of frustration at the national level, CID sees the commitments of Minister Hunt and his Department as very promising.
The Commission also heard from Dr Nigel Lyons, Deputy Secretary of NSW Health who talked about his agency’s current rollout of a statewide network of intellectual disability health services to provide specialist backup to hospitals and other health services.
Dr Lyons also outlined a range of other initiatives by NSW Health, including the production of The Essentials, a guide for public hospitals and other public health services about how they can improve capability in health care for people with intellectual disability. He acknowledged that it was up to Local Health Districts to decide what priority they give to action on The Essentials.
Earlier in the week, Jim Simpson had argued that implementation of The Essentials should be mandatory across Local Health Districts.
In line with the thinking of advocates around Australia, Jim also said that other States should take similar actions to the positive initiatives in NSW.
The other witness for the day was Graeme Head, the chief executive of the NDIS Quality and Safeguards Commission. He said that deaths of people with disability that occurred in connection with the provision of NDIS services had to be reported to the Commission. The Commission then has a range of actions it can consider taking, but can only focus on failings in NDIS services, not on failings in health services.
CID is very concerned about the limits on the deaths review role of the NDIS Commission compared with the comprehensive role that the NSW Ombudsman has had.
Find out more
- Minister Hunt’s media release about the $6.5m of new funding
- About The Essentials
- Our blog about the roadmap

Day seven – “The standard you walk past is the standard you accept.”
On day seven of the hearing the Royal Commission focussed on supported accommodation, and in particular the role of staff in ensuring good health care for people with intellectual disability.
Kathryn McKenzie, operations director at the Ageing and Disability Commission NSW, and Lynn Porter, official community visitor, spoke about the highly variable quality of health supports provided in group homes. They spelt out numerous problems, including:
- Disability staff wrongly assuming symptoms relate to a person’s the disability (a mistake we know doctors also often make)
- Inconsistent use of annual health assessments
- Health plans being out of date
- Failure to ensure that a trusted staff member takes an anxious person to a medical appointment
- People being chemically restrained when in fact they are in great pain from a dental problem
- Doctors chosen for staff convenience
One group home had engaged a male GP for women who had been victims of sexual abuse.
This evidence reinforced concerns that Jim Simpson had raised with the Royal Commission about:
- the NDIS Quality and Safeguards Commission not imposing clear standards on supported accommodation providers in relation to health care; and
- the loss of the regional specialist nurse positions that existed in NSW disability services to promote good health care for people in supported accommodation.
The Royal Commission also heard from an Adelaide mother and a Queensland sister about the inadequate health care received by their family members. They both emphasised the need to maximise the communication capacity of people with intellectual disability and the understanding of that communication by health care staff. Too often, health care staff do not even introduce themselves and explain their roles to people with intellectual disability, or help patients to fully understand proposed medical treatments.
The other witness on Wednesday was “Dr J”, a palliative care specialist who gave a number of alarming examples of cases where people with intellectual disability were not offered the treatment that they needed for cancer or life-threatening infections. False assumptions were made about whether the person could cope with treatment.

Day six – Meeting complex communication needs
Day six of the hearing started with Jacquie Mills from Perth telling the Royal Commissioners about issues for people who have complex communication needs, such as her son. Jacquie has been able to develop her son’s communication over time so that he can now indicate where he feels pain and answer questions on his iPad. But doctors have spoken about her son in front of him as if he didn’t have a life of his choosing. Doctors need training in working with people with complex communication needs.
As with other parents who have given evidence, Jacquie emphasised the challenges families can face in navigating the health system. Advocacy support can make all the difference.
CID Senior Advocate Jim Simpson emphasised the many barriers to good health care for people with intellectual disability, including the values of many health professionals.
To show the deep-seated history of this issue, he quoted from a 1988 discussion paper of the National Health and Medical Research Council, which looked at decisions about treatment of infants born with low birth weights. The paper did not just focus on the rights and interests of the infants, but also those of other people. It said “The dilemma is whether all such infants should receive all possible life-sustaining treatment for the sake of a few intact survivors.”
Jim said that we have made gains on values since then, but there is still a very major problem.
Jim emphasised the national disgrace that Australia has not comprehensively addressed the health inequalities of people with intellectual disability, despite these inequalities being well known since at least 1995.
He acknowledged valuable gains that have been made in NSW with intellectual disability health teams and the current movement towards a National Roadmap of action. He emphasised the range of actions required and the speed with which they should occur.
Nick Lennox, a researcher, GP and advocate from Queensland, presented Commissioners with a number of key priorities:
- Develop a strategy to drive take-up and quality of annual health assessments
- More comprehensive personal health records for people with intellectual disability
- Provide health care facilitators to people with complex health needs
- The need for specialists in intellectual disability medicine
- Recognise the role of people with intellectual disability as educators of health professionals
Read more in media stories on Tuesday’s hearing
- Intellectually disabled people ‘unsafe’ in hospitals, disability royal commission hears, ABC News
- Disability health care labelled a disgrace, AAP news

Day five – Powerful Indigenous input and a spotlight on oral health
Narelle Reynolds is a Wiradjuri woman with three adult children with Fragile X syndrome. She has worked as a nurse but has still found it very difficult to get the health and disability support that her children have needed.
Narelle said it’s a ‘double whammy’ in the health system being Aboriginal and having children with disability. She has found doctors dismissive and condescending. Getting cancer treatment for her son has been extremely difficult because doctors have not listened to her about the preparation her son needs to be comfortable in a hospital and accept treatment.
Scott Avery worked at First Peoples Disability Network and is now a university lecturer. He outlined four key barriers to health care for indigenous people with disability:
- Getting a diagnosis, as Indigenous people don’t take a ‘deficit’ approach to disability.
- Negative assumptions about a person’s decision-making capacity.
- Diagnostic ‘overshadowing’. For example, where a person is assumed to be drunk rather than have a disability or be ill.
- Rationing of health care resources. For example, an Aboriginal man discharged from hospital after surgery to sleep rough.
Sabrina Monaghan spoke about her son with autism who understands plain English but is mostly non-verbal and communicates in other ways. Her son has had an excellent long-term relationship with his neurologist but all sorts of trouble getting the right dental care. A ‘special needs’ dental clinic asked no questions about her son’s support needs or how they could make reasonable adjustments. Understandably, her son would not open his mouth. Finally, he is on the waiting list for the right examination and treatment but there could be a two-year wait.
Sabrina said that dental clinics should offer comfortable environments through soft lighting, relaxing music, familiar items and pre-planning to meet an individual’s sensory needs.
Nathan Despott from Inclusion Melbourne and dentist Richard Zylan talked about valuable work they are doing with the Australian Dental Association, including producing an oral health guide for people with disability and their families and a guide on inclusive practice for dentists.
Find out more
- Inclusion Melbourne’s oral health resources
- Scott Avery’s book Culture is Inclusion

Day four – “Just listen to us!”
On Friday, the Royal Commission heard it straight from a woman with intellectual disability and three parents.
Former CID vice-chair Christine Regan gave evidence with her daughter Erin Sheevy. When Erin was born, the hospital advice was “We think you should send this baby to a place where it can be looked after because you can’t!” The paediatrician gave fundamentally wrong advice that Erin had only one in five chance of surviving heart surgery. Another specialist walked out of his own office when Christine questioned his advice.
When Erin was a young woman she had a stroke but was not offered the usual rehabilitation. When Christine press this, the response was, “She has Down syndrome. How hard are you going to try?”
Many years on, Erin is now living a full life and working in a coffee shop.
Christine emphasised that doctors should not be providing their social opinions. They should stick to medical opinions.
Tara Elliffe is a member of CID and also works at the NSW Ombudsman. Tara told the Commissioners how doctors should communicate with people with intellectual disability. They should listen carefully, use simple words and pictures and easy read. They should talk to the person not their parents. Tara concluded, “just listen to us!”
Kim Creevey from Queensland told the story of her son Harrison who had quadriplegia and a brain injury from an illness as a small child. The family had trouble over the years in getting the healthcare that Harrison needed. One paediatrician said to Kim in front of Harrison, “How much more money are we going to spend on him, keeping him alive?” Harrison understood what the doctor said.
When Harrison was 17, Harrison was very sick in hospital but there were failures in his care and he died. Kim said that Harrison’s death was preventable. “He didn’t need to die.”
Media stories
- Hear Tara and Margot Elliffe, Toni Mitchell and Perth parent Jaqui Mills on Julian Morrow’s Sunday morning radio show.
- Read more about Kim Creevey’s evidence from ABC News.
- See also a story from The Guardian about the first week at the Royal Commission.
- To also an SBS news report about the week’s evidence.

Day three – Hearing from the doctors
On day three the Royal Commission heard from three eminent doctors.
Julian Trollor talked about his landmark research on the health of people with intellectual disability and more recent research on health of people with autism. Julian said that the health needs of people with intellectual disability and autism are not being met at any level or component of the health system.
People with autism have extremely high rates of suicidal thinking, but are not mentioned in the National Suicide Strategy.
There are probably 400 people with intellectual disability dying preventable deaths in Australia every year.
Julian agreed with Commissioner Atkinson that an incremental response to these health disparities was clearly inadequate. He said we need to start from a human rights framework and take comprehensive action to implement it.
Jackie Small is a developmental paediatrician and President of the Australian Association of Developmental Disability Medicine. She is working in one of the new intellectual disability health teams in NSW.
In 2017, NSW Health also developed The Essentials framework for hospitals and other State health services to build their capability in working with people with intellectual disability. Jackie is not aware of any Local Health District that is implementing The Essentials.
Jackie called for a national strategic plan on the health of people with intellectual disability and said that the current draft National Roadmap for Improving the Health of Australians with Intellectuals Disability has potential to take this role.
Early in the day the Commission heard from Professor Steve Leeder, a public health specialist and former Dean of Medicine at Sydney University. Steve has always had a strong focus on equity in health care and has supported CID’s health campaigns. Professor Leeder provided the Commissioners with an outline of the Australian health system.
Find out more

Day Two – “The first ultrasound set the tone for his life”
Yesterday, The Royal Commissioners heard harrowing evidence from two mothers whose sons with Down syndrome have been woefully failed by the health system.
Toni Mitchell from Toowoomba gave evidence with her son Joshie. She said that, when she had her first ultrasound, the technician just ran out of the room. An older man came in and said to her “He’s got Down syndrome. Here’s your appointment for a termination.”
Toni said she has had to justify Joshie’s life over and over. Joshie had repetitive bad experiences in public hospitals including the wrong surgeries being done. A gastroenterologist couldn’t see past Joshie’s Down Syndrome and he suffered 14 years of agony before getting the proper diagnosis and treatment. More recently, Joshie has gone to a private hospital and received good treatment.
Rachel Browne from Bathurst told the Commissioners about her son Finlay, a name which means ‘fair-haired warrior’, and that is what he was every day of his life. Despite being a nurse herself, Rachel had ongoing problems getting the right healthcare for Finlay, especially at times when she had to take him to the emergency department at the local hospital. An emergency doctor described him as “a grizzly child with Down Syndrome”.
The events of 30 September 2016 stay vividly etched in Rachel’s memory. Finlay was in terrible pain and vomiting and saying, “Mum please help me!” On arriving at the emergency department, Finlay collapsed and the triage nurse rolled her eyes. It was 45 minutes before a doctor saw Finlay. There was a lack of urgency or action. Eventually, a CT scan showed a bowel obstruction. After late night surgery, Finlay was flown to Westmead Children’s Hospital the next morning. After 71 days, 12 surgeries and excellent care at Westmead, Finlay died with all his family beside him.
You can read more about Rachel’s evidence at the ABC News website.

Day One – “We want R-E-S-P-E-C-T !”
The Disability Royal Commission hearing on health started with powerful evidence from people with disability and their families.
CID member Kylie Scott told the Commissioners how doctors should work with people with intellectual disability. Ask short questions in plain English. Be patient. We want R-E-S-P-E-C-T, Kylie said. It makes it a lot easier when she trusts the doctor.
Rebecca Kelly from Tasmania talked about the great challenges she has faced in getting the right healthcare for her “all-round delightful little boy” Ryan, who has Down syndrome and complex health care needs. Ryan suffers from ongoing trauma because doctors have not been open to how he expresses pain. “Look, it’s not even hurting him”, said a doctor. WRONG. Ryan just shows pain differently and needs medication to help him deal with medical procedures.
Rebecca said that despite her university education and strong advocacy skills, it is so hard to get the right healthcare for Ryan. “What on earth happens to kids whose parents don’t have my advantages?”
Rebecca stressed that the attitude of doctors is key. It is a really bad start if a doctor says “We’re really sorry but your child has Down Syndrome.” If doctors see disability as a tragedy, it affects their whole mindset.
Earlier, Commission Chair Ronald Sackville opened proceedings saying that the neglect and abuse experienced by people with cognitive disability in the health system should “shock the conscience of all Australians.”
Jack Kelly and Justine O’Neill from CID talked about how Jack goes about making his own life decisions and about the fundamental changes that are needed so that people with intellectual disability are routinely supported to make their own decisions rather than having decisions made about them. If doctors don’t listen to people, things go wrong!
There was a lot of media interest on day on of the hearings. Here is a selection of items that featured members of the CID team:
- Disability Royal Commission resumes hearings in Sydney, on ABC radio, in which our CEO Justine O’Neill and mother Rebecca Kelly talk about why it is so important that our health system improves for people with intellectual disability.
- Making the Disability Royal Commission accessible for witnesses, an ABC radio report about making the Commission accessible, featuring our Chairperson Shu Hua Chan.
- Read Royal commission to hear ‘shock’ concerns from Australians with cognitive disabilities, SBS News, 18 February.
About the Sydney Hearing
The Disability Royal Commission is holding Public Hearings across Australia. There have been Public Hearings in Melbourne and Brisbane.
The Sydney public hearing focusses on health issues, and runs until 28 February.


 1800 424 065
1800 424 065